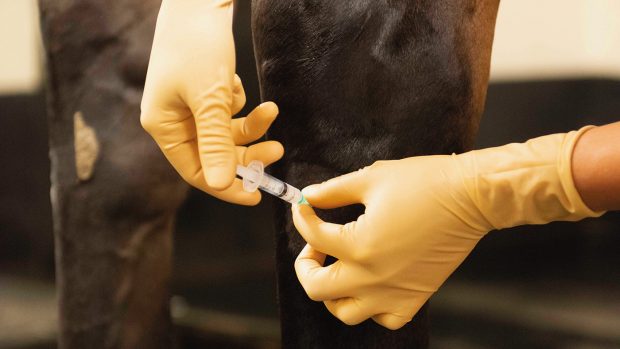
Desensitising part of a limb with anaesthetic may be necessary to localise the source of pain, as Dr Liz Barr explains
When there is no obvious swelling, heat or discomfort in the leg of a lame horse, the best option to localise the pain causing the lameness is to use diagnostic analgesia — which are commonly described as nerve blocks in horses. Blocking is also useful when a horse has multiple areas of swelling, some of which may be old, to confirm whether a particular finding on clinical examination is significant.
A nerve block involves injecting local anaesthetic around nerves at specific points on the limb, to desensitise various regions.
Local anaesthetic stops nerve signals to the brain; while the horse cannot feel pain after a nerve is successfully blocked, he can feel some pressure or movement.
The aim is to deposit the anaesthetic solution without touching the nerve itself with the needle, as this can result in a very quick and dangerous reflex kick. The anaesthetic can also be injected directly into joints or tendon sheaths to abolish pain associated with these structures.
How nerve blocks in horses work
The procedure takes place under veterinary guidance, at home or at a clinic. The horse is first watched in action to determine the baseline level of lameness. Some horses may not be obviously lame when trotted up in hand, or may have more general poor performance issues or problems that affect certain movements only. These patients will also need to be seen working under saddle.
The predominantly lame leg is then identified, but bear in mind that some horses will be lame in multiple legs. Others may merely appear so as a result of compensatory lameness, which arises from altered loading of limbs due to pain in one of them.
Blocking generally starts with an injection at the bottom of the affected limb, after which the horse is viewed in motion again.
Sequential nerve blocks are performed, working upwards, until the horse becomes sound or shows a significant improvement in the level of lameness — indicating the origin of the pain.
The exact cause can then be identified by appropriate imaging such as X-ray, ultrasound, MRI or CT, to reach an accurate diagnosis and formulate a treatment plan.
A more targeted approach may be preferable when blocking a hind limb to avoid the need for excessive injections, particularly in a sharp horse or known kicker.
The bottom hock joints are a common site of pain and lameness, so I often start by blocking these in a middle-aged or older horse with no palpable abnormalities. If the lameness does not improve, I go back and start at the bottom of the limb. If it does improve, however, I’ve managed to avoid up to four of these lower blocks.
Risks and limitations of nerve blocks in horses
Putting a needle into a horse’s leg, particularly a hindleg, is risky for a vet. There’s the added danger that a sudden kick or a quick move can result in the needle breaking off under the horse’s skin. Experienced handling can reduce risk, along with measures such as fitting the horse with a twitch, lifting another of his limbs, distracting him with food or using short-acting sedation.
If there is any suspicion that lameness is caused by a non-displaced fracture of a limb, blocking should be avoided. Removing the pain and repeatedly trotting and lungeing the horse can result in a catastrophic displaced fracture.
Vet and owner must recognise the limitations of nerve and joint blocks, and confusing information that may be thrown up.
Joint blocks can abolish pain in adjacent areas, creating misleading results. A common occurrence is a “cross-over block”, such as an injection into the bottom hock joint that also removes pain from the proximal suspensory ligament region. For this reason, it is routine to scan the proximal suspensory ligaments as well as X-raying the hocks of horses that go sound after this block.
Another shortcoming is that joint blocks may not abolish all the pain, although the joint is the problem. An example is persistent lameness in the subchondral bone, directly below the cartilage surface of the joint, where the anaesthetic solution is inadequately absorbed. There can also be issues within complex joints such as the stifle, where various joint compartments may not “communicate” to let the anaesthetic permeate the whole area.
Nerves can also be blocked incompletely, resulting in continued transmission of some pain and a response that is not as expected. Conversely, the anaesthetic sometimes diffuses up the limb — it may appear from the results of the blocking pattern that the pain is coming from the foot, but the anaesthetic has risen and blocked out fetlock joint pain.
Procedure prep
An additional risk is infection, usually of a synovial structure (a fluid-filled joint cavity). This can be minimised by first scrubbing the injection site with an antiseptic solution before applying surgical spirit. Clipping hair or feathers will enable easier palpation of the anatomy and more accurate needle placement, although this can still be difficult in very thick-skinned cob types and heavy breeds.
No other preparation should be necessary. Where a leg has been subject to multiple injections, applying a stable bandage overnight is a good precaution against swelling.
How much do nerve blocks in horses cost?
A number of nerve or joint blocks may be needed to abolish lameness, each costing £45-90 depending upon on the level of complexity (price correct as of early 2019). Once the service fee for lameness evaluation is added, plus local anaesthetic solution costs of around £12 per 10ml bottle (with 5ml being required to block a foot and 60ml for a stifle joint), costs can soon escalate.
Despite the expense and the inherent risks, diagnostic analgesia is of utmost importance in lameness diagnosis. Without obvious clinical findings, it is the only way to identify the source of pain categorically, and accurately diagnose and treat the issue.
Nerve block case study: ‘it was worth persevering’
Dutch dressage mare Peaches first attended the Bell Equine Vet Clinic in May 2016, with right forelimb lameness. Nerve blocks of the lowest parts of the limb failed to alter the lameness, but she came sound after a below-the-knee nerve block.
Subsequent ultrasound scans revealed damage to the proximal suspensory ligament, so Peaches was rehabilitated accordingly and regained soundness. Repeat ultrasound scans looked encouraging, but the lameness returned when she started full work the following spring and the ultrasound appearance seemed to have deteriorated. After trying unsuccessfully to put her in foal, her owners gave her the rest of the year off.
Last April, Peaches was reassessed to see if she would be capable of some light hacking. She remained lame on the right fore, although ultrasound scans of the proximal suspensory ligament showed no real reason for this. However, the 14.2hh mare came sound after an abaxial sesamoid nerve block — an injection of local anaesthetic above the fetlock joint. This indicated that the previous suspensory injury was not the reason for the residual lameness.
More specific blocks were then performed. Diagnostic imaging of the lower limb then enabled diagnosis of a synovial ganglion cyst (a fluid-filled lesion) of the digital flexor tendon sheath, along with mild arthropathy (joint disease) of the distal interphalangeal (coffin) joint. Once the digital flexor tendon sheath was medicated with hyaluronic acid, Peaches, now 15, regained soundness.
“It was worth persevering,” says her owner Rosemarie Lovegrove. “My daughter Bryony is now at university, so Peaches is my ‘happy hacker’, which is all we really wanted.”
First published in Horse & Hound; 14 February 2019
You may also be interested in…

Lameness in horses: what every owner needs to know

The lameness work-up: what it is and what it can achieve

Degenerative Joint Disease (DJD) / arthritis in horses: all you need to know

Subscribe to Horse & Hound this spring for great savings
Horse & Hound magazine, out every Thursday, is packed with all the latest news and reports, as well as interviews, specials, nostalgia, vet and training advice. Find how you can enjoy the magazine delivered to your door every week, plus options to upgrade your subscription to access our online service that brings you breaking news and reports as well as other benefits.